RCOphth is continuing to assess and monitor the pandemic and to publish real-time guidance and advice for ophthalmology services during COVID-19.
Healthcare services are now planning how to move from full lockdown with severely restricted activities to re-opening services. However, there will be continuing and potentially variable levels of restrictions for potentially many months. Issues related to physical distancing and infection control procedures are also likely to limit available capacity. There will need to be a phased approach and a continuing requirement to prioritise care.
Our resources include guidance and a joint vision of ophthalmic services during and beyond COVID-19. We are working with sub-specialty groups, The College of Optometrists, NHS England & Improvement and various charities.
RCOphth Response to COVID-19
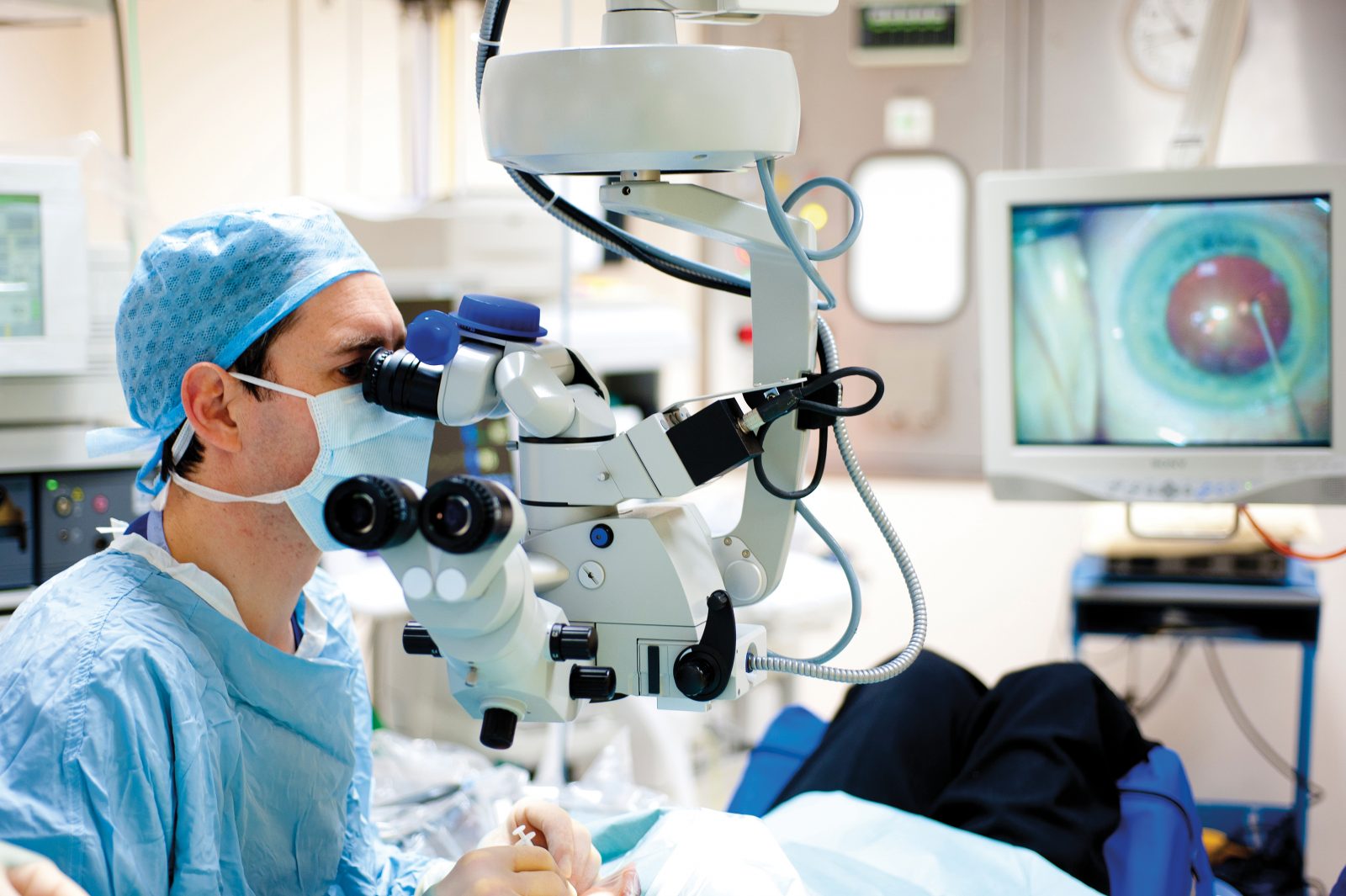
Mike Burdon, former RCOphth President, discusses with Melanie Corbett, Chair of Education, the response to the COVID-19 epidemic from RCOphth on streamlining outpatient appointments and surgery using what we have learned during the crisis.